Herniated Disc Treatment: What Actually Helps Back Pain, What Doesn’t, and How to Recover Safely
A clear, research-backed guide to herniated disc treatment, explaining what truly helps recovery, what often makes symptoms worse, and how to move forward with confidence.
2/6/20266 min read


Herniated Disc Treatment:
What Helps & What Doesn't, Explained Without the Fear
A herniated disc has a way of hijacking your thoughts. The pain can be sharp, strange, and frightening—sometimes in your back, sometimes racing down your leg—and the diagnosis alone can make everyday movement feel risky. Many people wonder the same thing in those first confusing weeks: Is this something that heals on its own, or am I going to need serious intervention to feel normal again?
The reassuring truth is that most herniated discs improve without surgery. The frustrating part is that not everything marketed as “treatment” actually helps—and some well-intended choices can slow recovery. Understanding the difference is what gives people back control.
How a herniated disc actually happens and how it’s diagnosed
Your spine is made up of stacked bones (vertebrae) cushioned by discs. Each disc has a tougher outer ring and a softer, gel-like center. Over time (or occasionally with sudden strain) the outer ring can weaken. When pressure builds, part of the softer center can push outward. That’s a herniated disc.
This doesn’t always happen because of one dramatic moment. More often it’s a combination of age-related wear, repetitive movement, prolonged sitting, or cumulative stress. Some people don’t feel a thing; others feel pain because the bulge irritates a nearby nerve root. When that nerve irritation causes pain, tingling, numbness, or weakness down an arm or leg, doctors call it radiculopathy. In the lower back, that often shows up as sciatica—pain that travels through the buttock and down the leg.
Diagnosis usually starts with a physical exam and detailed symptom history, not imaging. Clinicians look for nerve-related signs like altered reflexes, muscle weakness, or pain patterns that match specific nerve roots. Imaging such as MRI is typically reserved for cases where symptoms are severe, worsening, long-lasting, or when procedures like injections or surgery are being considered. Both the American Association of Neurological Surgeons (AANS) and guidelines published in family medicine journals emphasize that early imaging often increases anxiety without changing treatment for most people.
In other words, treatment decisions should be guided by how you’re functioning—not just what a scan shows.
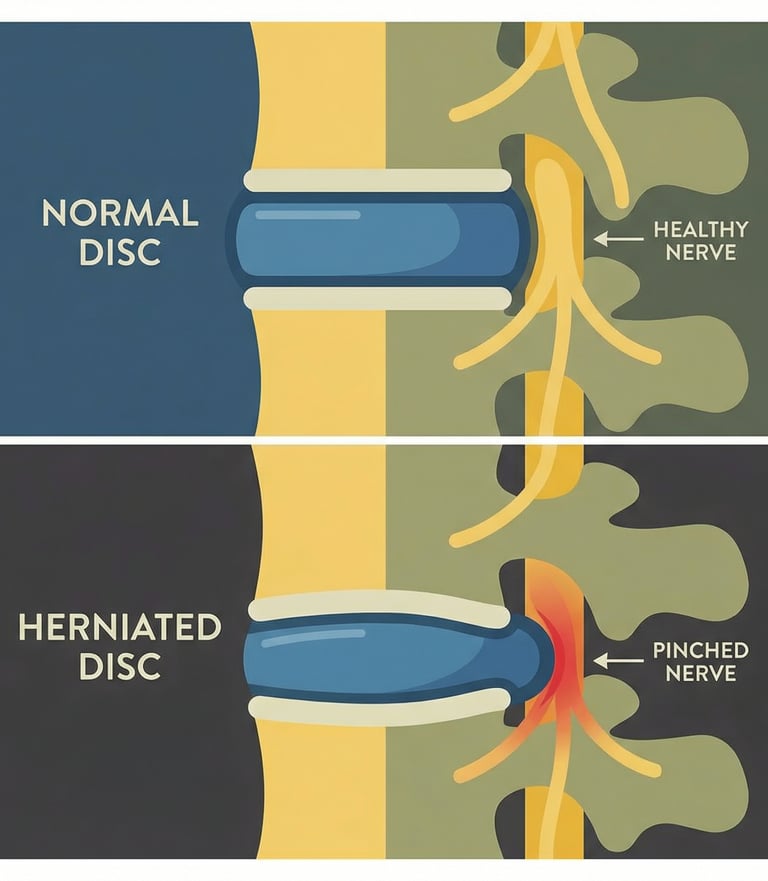
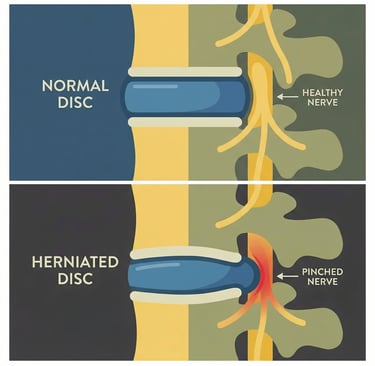
What consistently helps herniated discs recover
Your recovery to-do list
The most effective treatments are usually not flashy. They work because they support the body’s natural healing process while keeping you functional and confident enough to move.
One of the most important factors is time combined with the right amount of activity. According to the AANS, the majority of people with disc herniation experience significant improvement within weeks to months, and about 90 percent recover without surgery. Walking and gentle daily movement are encouraged early, while prolonged bed rest is discouraged because it slows recovery and increases stiffness and fear around movement.
This aligns with findings from large evidence reviews conducted by the Cochrane Collaboration, an international nonprofit group known for rigorously evaluating medical research. Their analyses have shown that staying active leads to better outcomes than extended rest for acute low back pain and sciatica.
Another cornerstone of recovery is symptom-guided physical therapy. Physical therapists who specialize in spinal conditions aim to calm nerve irritation, restore confidence in movement, and gradually rebuild strength. One commonly used framework is Mechanical Diagnosis and Therapy (often called the McKenzie method). Research published in peer-reviewed journals has shown that, when appropriately matched to the patient, this approach can reduce pain and disability, particularly in the earlier stages of disc-related pain.
Medications can help—but primarily as a short-term support. Anti-inflammatory medications may reduce pain enough to keep people moving, which matters more than pain elimination alone. Oral steroids are sometimes prescribed, but a randomized clinical trial published in JAMA found that while steroids slightly improved function, they did not meaningfully reduce pain. They are not a cure, just a possible bridge.
Epidural steroid injections can be helpful for people with persistent nerve pain, especially leg-dominant symptoms that make movement difficult. High-quality systematic reviews published in neurology journals have found strong evidence that certain types of epidural injections can reduce radicular pain from disc herniation in the short term. These injections don’t “fix” the disc; they reduce inflammation around the nerve so rehabilitation and natural healing can continue.
Surgery is typically reserved for people whose pain remains disabling despite conservative care, or who develop significant neurologic deficits. Large, long-term studies, including randomized trials published in The New England Journal of Medicine and JAMA, show that surgery often provides faster pain relief—but many people who don’t have surgery improve as well, just on a slower timeline. Surgery can be the right choice, but it’s rarely the first or only path to recovery.




Do: Walking and gentle movement
Do: Symptom guided physical therapy


Do: Consult with a doctor
What often doesn’t help—and what to try instead
Replace don't-dos with these helpful tips
Prolonged bed rest is one of the most common missteps. While short rest may be necessary during severe flare-ups, staying inactive for days or weeks leads to muscle deconditioning and increased pain sensitivity.
Instead try: gentle walking, frequent position changes, and light activity that does not increase nerve symptoms over the next day.
Getting immediate imaging “just to know” is another common trap. MRI findings are common even in people without pain, and seeing disc changes early can increase fear without improving outcomes.
Instead try: a structured evaluation focused on symptoms and function, with imaging reserved for persistent or worsening cases.
Aggressive stretching into nerve pain is also problematic. Sharp, electric, or shooting sensations are signs of nerve irritation, not tight muscles being “released.”
Instead try: movements that decrease leg pain and keep symptoms closer to the back, guided by a clinician when possible.
Some people pursue repeated spinal manipulation with the idea that the disc needs to be “put back in place.” Research comparing different manual therapy approaches has shown that gentler mobilization combined with nerve-friendly movement often leads to better outcomes than forceful manipulation alone.
Instead try: care focused on restoring movement tolerance, strength, and functional confidence rather than chasing structural correction.
Finally, focusing only on the disc itself can limit recovery. The hips, core musculature, walking tolerance, sleep quality, and stress response all influence pain.
Instead try: building overall capacity with gradual strength training, aerobic activity, and sleep support alongside targeted care.


Swap prolonged rest with light activity


MRIs can be stressful and costly.


Avoid aggressive stretching. Try to restore movement tolerance slowly.
When waiting is not the right move
Although most herniated discs improve, some symptoms require urgent evaluation. Sudden or progressive weakness, loss of bowel or bladder control, or numbness in the saddle region are red flags that warrant immediate medical attention, as emphasized by the AANS.
Practical, research-supported ways to support healing
People recover best when they monitor how activities affect them over time. A simple rule many clinicians use is the 24-hour response: if pain is significantly worse the next day, scale back. If symptoms are stable or improving, continue.
Walking is consistently recommended because it maintains circulation, spinal movement, and confidence without excessive load. Gradually rebuilding strength—especially through the hips and trunk—helps reduce stress on the spine over time.
When injections or medications are used, they work best as tools that allow progress rather than replacements for rehabilitation. Surgery remains an option when symptoms demand it, but it is rarely the only chance for improvement.
Calmer, smarter care leads to better outcomes
A herniated disc diagnosis can sound intimidating, but the research paints a hopeful picture. Most people recover with time, thoughtful movement, and symptom-guided care. The treatments that help the most are rarely dramatic; they’re steady, evidence-based, and focused on restoring function rather than eliminating discomfort overnight.
Understanding what truly helps—and avoiding what doesn’t—puts recovery back in your hands. And for those navigating this process with questions, setbacks, or uncertainty, the Bounce Back community exists to offer clarity, support, and real-world guidance from people who understand the path forward.
